Ebener, S., Barnowski, S., Wotzkow, C., Marti, T.M., Lopez-Rodriguez, E., Crestani, B., Blank, F., Schmid, R.A., Geiser, T., Funke, M.: Am J Physiol-Lung C. 2017;312(1):L42-55
To access the full article, click here:

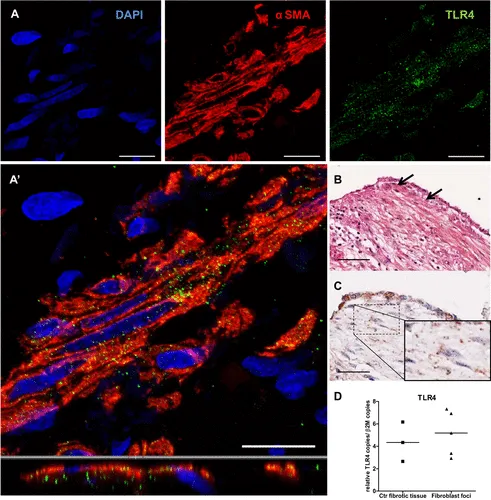
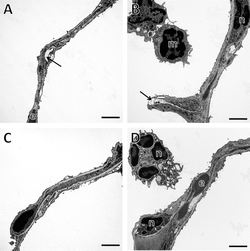
Idiopathic pulmonary fibrosis (IPF) is a devastating lung disease with a median survival of 3 yr. IPF deteriorates upon viral or bacterial lung infection although pulmonary infection (pneumonia) in healthy lungs rarely induces fibrosis. Bacterial lipopolysaccharide (LPS) activates Toll-like receptor 4 (TLR4), initiating proinflammatory pathways. As TLR4 has already been linked to hepatic fibrosis and scleroderma, we now investigated the role of TLR4 in IPF fibroblasts. Lung tissue sections from patients with IPF were analyzed for TLR4 expression. Isolated normal human lung fibroblasts (NL-FB) and IPF fibroblasts (IPF-FB) were exposed to LPS and transforming growth factor-β (TGF-β) before expression analysis of receptors, profibrotic mediators, and cytokines. TLR4 is expressed in fibroblast foci of IPF lungs as well as in primary NL-FB and IPF-FB. As a model for a gram-negative pneumonia in the nonfibrotic lung, NL-FB and IPF-FB were coexposed to LPS and TGF-β. Whereas NL-FB produced significantly less connective tissue growth factor upon costimulation compared with TGF-β stimulation alone, IPF-FB showed significantly increased profibrotic markers compared with control fibroblasts after costimulation. Although levels of antifibrotic prostaglandin E2 were elevated after costimulation, they were not responsible for this effect. However, significant downregulation of TGF-β receptor type 1 in control fibroblasts seems to contribute to the reduced profibrotic response in our in vitro model. Normal and IPF fibroblasts thus differ in their profibrotic response upon LPS-induced TLR4 stimulation.